Mobile App Cuts Skin Cancer Referrals in Half, British Trial Shows
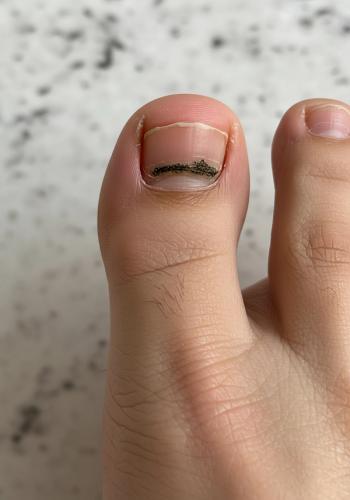
The Map My Mole app provides patients with a small lens attachment for their phones to capture high-quality images of concerning skin spots. These images are then uploaded for assessment by consultants.
A mobile app designed to help detect potential skin cancer has reduced hospital referrals by more than 50% in a trial at three primary care clinics in Britain's National Health Service.
The Map My Mole
The system works by giving patients a small lens attachment for their phones to capture high-quality images of concerning skin spots. These images are then uploaded for assessment by consultants, bypassing traditional referral pathways for many benign conditions.
"In the three sites participating, we have reduced GP-to-hospital referrals by over 50%," said Dr. Toby Nelson, a dermatologist involved in the trial, to the
Another location that participated in the trial reported a significant drop in further referrals — only 10% of the 400 patients evaluated were sent on for additional review.
Non-melanoma skin cancer is the most common type of cancer in the United Kingdom, though many cases are not included in national cancer statistics due to differences in how they’re recorded and treated, according to
While most cases are treatable when detected early, delays in diagnosis can lead to more complex care and poorer outcomes. The growing burden on dermatology services has fueled interest in technologies that can support earlier identification and reduce unnecessary specialist referrals.
Artificial intelligence is improving skin cancer detection, with studies showing a 15% to 20% improvement in prediction accuracy. In the United States, the FDA last year
In a pivotal study led by the Mayo Clinic, the device, called DermaSensor, showed a 96% sensitivity rate across all skin cancer types and cut the rate of missed cancers in half. In a companion clinical utility study with 108 physicians, the DermaSensor device was found to decrease the number of missed skin cancers by half (from 18% to only 9%).
In the United States, one out of five Americans will have had some type of skin cancer by the age of 70. The annual cost of treating skin cancers in the United States is estimated at $8.1 billion, with an estimated 5.5 million new cases each year.
Such technologies have broader implications for dermatology services, where specialists currently dedicate significant time reviewing referrals that often prove benign. By reducing unnecessary specialist visits, consultants could potentially redirect resources to patients with chronic skin conditions.
“If we can reduce unnecessary referrals, consultants will have more time to see patients with eczema, acne, and psoriasis, who currently face waits of six to 18 months,” Dr. Nelson said.
Newsletter
Get the latest industry news, event updates, and more from Managed healthcare Executive.